Chiari and Syringomyelia 101
by John Oró, MD
A Brief Look at Neuroanatomy
The brain is enclosed and protected by a rounded skull made of rigid bone. The bottom of the skull contains multiple openings called foramen through which nerves and blood vessels pass. The inside of the skull, called the intracranial space, is partly separated into two compartments by a tent like structure called the tentorium. The large compartment above the tentorium is called the supratentorial compartment and the compartment below the tentorium is called the infratentorial compartment. (Supra means above, and infra means below.) Most doctors call the infratentorial compartment the posterior fossa.
The supratentorial compartment contains the two halves of the cerebrum known as cerebral hemispheres. The hemispheres come together in a deep central area called the diencephalon. Through an opening in front of the tentorium, the diencephalon connects to the brain stem. On the back of the brainstem sits the cerebellum. The brain stem continues through an opening at the bottom of the skull, called the foramen magnum, and connects with the spinal cord. The spinal cord runs in the spinal canal.
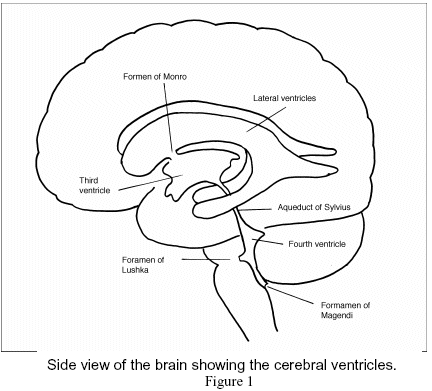
There are four cavities filled with spinal fluid within the brain called ventricles. [see Figure 1] Two large C-shaped ventricles, called the lateral ventricles, are located within the cerebral hemispheres and are connect by two small tunnels (the foramen of Monro) to the third ventricle. From the third ventricle spinal fluid flows through a small tunnel known as the Aqueduct of Sylvius to the fourth ventricle which is located between the brain stem and the cerebellum. Spinal fluid flows out of the fourth ventricle through three openings: two openings at the side of the fourth ventricle called the foramen of Luschka and one at the bottom of the fourth ventricle called the foramen of Magendie. From these three foramina spinal fluid flows out of the ventricular system to the surface of the brain as well as down the spinal canal and back up. Spinal fluid is created by a tuft of vascular tissue called the choroid plexus that is present within each ventricle. With every heartbeat, blood passing in the choroid plexus is filtered to create a clear colorless fluid that looks like water called cerebral spinal fluid or CSF. The spinal fluid flows down through the ventricles, exits the through the three openings of the fourth ventricle, and flows around the brain and spinal cord. The spinal fluid is taken back up in the vascular system through a large vein located at the top of the brain called the sagittal sinus. By way of special connections called arachnoid granulations, the spinal fluid drains into the sagittal sinus. Here it becomes part of the blood that drains through the jugular veins to the heart. With each heartbeat, a small amount of spinal fluid is created inside the ventricles at the same time a small amount is taken up by the veins, keeping the system in balance.
The spinal fluid helps cushion the brain from injury. The space around the surface of the brain and within the spinal canal that contains spinal fluid is called the subarachnoid space. Partial membranes of a thin veil-like material called the arachnoid divide the subarachnoid space, much like the baffles in some waterbeds that limit large wave action. The resulting pockets are called cisterns. An important subarachnoid cistern, the cisterna magna, is located at the bottom of the skull. (The word magna, which means great or large in Latin, serves to remind us that it is the largest cistern in intracranial space.) The cisterna magna is important because most of the spinal fluid flowing from the ventricles drains into it on its way to the spinal canal and over the surface of the brain. Crowding of the cisterna magna, such as in the Chiari I malformation, can block the normal flow of spinal fluid.
As noted above, the posterior fossa contains three important neurological components: the brain stem, cranial nerves, and cerebellum. The brain stem, a very vital area of the brain, contains the nerve centers (nuclei) that control eye movements, feeling and movement of the face, hearing, swallowing, shrugging the shoulders, and movement of the tongue. From these nuclei run the cranial nerves that travel through small foramina (openings) at the bottom of the skull to and from their area of activity. The brainstem also has nerve centers that controls heart and breathing functions. The cerebellum, attached to the back of the brainstem, regulates coordination and fluidity of movement.
Disorders of the cerebellum can include unsteady gait, balance problems, and difficulty with fine motor tasks. Like the cerebrum, the cerebellum is divided into two hemispheres. At the bottom of each cerebellar hemisphere is the tonsil. These tonsils are different from those located in the throat.
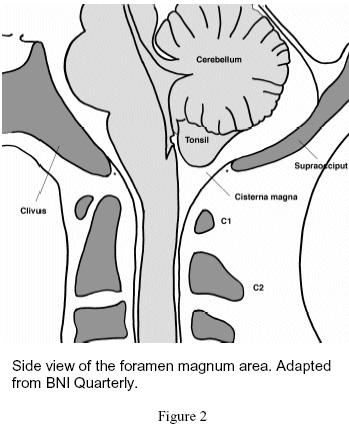 Figure 2 shows a side view of a normal posterior fossa. The triangular shaped bone in front of the brain stem is called the clivus. The skull bone behind the cerebellum is called the supraocciput. The tent like structure above the cerebellum is the tentorium. We can also see the foramen of Magendi, one of the three outlets from the fourth ventricle located just in front of the tonsil, and the cisterna magna. If we draw a line starting at the lower end of the clivus to the lower end of the supraoccitput bone (dots on the figure), we are outlining the large opening at the bottom of the skull called the foramen magnum. We can also see that the brain stem becomes the spinal cord at about the level of the foramen magnum. Within the spinal cord run nerve fibers that control movement of the arms, trunk, legs and bowel and bladder function. Nerves for feeling from the body run up the spinal cord. The upper bones (vertebrae) of the spine can also be seen. The upper most is called cervical one, or C1 for short, and the second one called cervical two (C2) .
Figure 2 shows a side view of a normal posterior fossa. The triangular shaped bone in front of the brain stem is called the clivus. The skull bone behind the cerebellum is called the supraocciput. The tent like structure above the cerebellum is the tentorium. We can also see the foramen of Magendi, one of the three outlets from the fourth ventricle located just in front of the tonsil, and the cisterna magna. If we draw a line starting at the lower end of the clivus to the lower end of the supraoccitput bone (dots on the figure), we are outlining the large opening at the bottom of the skull called the foramen magnum. We can also see that the brain stem becomes the spinal cord at about the level of the foramen magnum. Within the spinal cord run nerve fibers that control movement of the arms, trunk, legs and bowel and bladder function. Nerves for feeling from the body run up the spinal cord. The upper bones (vertebrae) of the spine can also be seen. The upper most is called cervical one, or C1 for short, and the second one called cervical two (C2) .
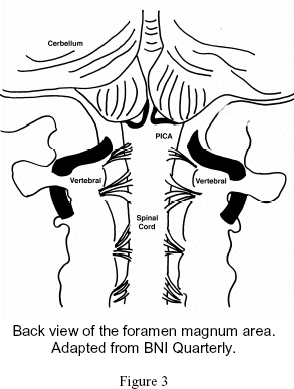 Figure 3 shows the area of the foramen magnum from behind. The cerebellar tonsils at the lower part of each cerebellar hemispheres can be seen. Also visible is the lower end of the brain stem and the spinal cord. Small nerves enter and leave the surface of the spinal cord. The large arteries seen running through the C1 and C2 vertebrae, called the vertebral arteries, deliver blood to the brain stem and cerebellum, and to a portion of the cerebral hemispheres. An important branch of each vertebral artery can be seen as small loops just below each tonsil. These are called the posterior inferior cerebellar arteries, called PICA for short.
Figure 3 shows the area of the foramen magnum from behind. The cerebellar tonsils at the lower part of each cerebellar hemispheres can be seen. Also visible is the lower end of the brain stem and the spinal cord. Small nerves enter and leave the surface of the spinal cord. The large arteries seen running through the C1 and C2 vertebrae, called the vertebral arteries, deliver blood to the brain stem and cerebellum, and to a portion of the cerebral hemispheres. An important branch of each vertebral artery can be seen as small loops just below each tonsil. These are called the posterior inferior cerebellar arteries, called PICA for short.
Figure 4 is a cross section of the spinal cord. The fibers in the spinal cord are organized in a very specific way. Fibers for feeling and movement run together in nerve highways called tracts. The spinal nerves bring sensory information, such as pain and temperature, in to the spinal cord and send information out to muscles are like on and off-ramps on a major highway. The spinal nerves merge in to the nerve tracts heading up of down in the spinal cord. Two main nerve tracts carry sensation from the body up to the brain: the dorsal columns and the spinothalamic tract. The dorsal columns (DC) located at the back of the spinal cord bring information from the body, arm and legs about the position of the body and vibration. The spinothalamic tract (ST), located at the front of the spinal cord, brings up information about pain and temperature. The corticospinal tracts (CTS) are composed of motor nerves cells that control movement.
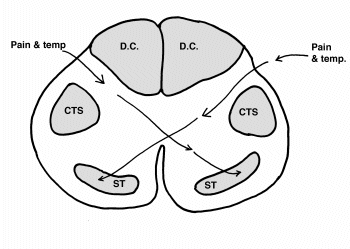
Here the story gets a bit more complicated. The feeling fibers coming in from the spinal nerves enter the spinal cord on its back surface. They connect to the spinothalamic fibers that then travel to the front and opposite side of the spinal cord before they enter the spinothalamic highway up to the brain. Thus, the fibers bringing information in about pain and temperature of the right side of the body cross to the left side of the body cross to the right side of the cord. They cross is near the center of the spinal cord. Syringomyelia often starts at the center of the spinal cord. Thus fibers carrying information about pain and temperature are among the first affected in patients with syringomyelia. As the syrinx enlarges, it can affect other tracts and result in weakness and problems walking. Often, one side is more affected than the other. The mix of symptoms depends on which type of fibers and nerve cells are affected.
Discovery of the Syringomyelia & Chiari Malformations
1827, Charles Prosper Ollivier dAngers, published an article about disorders of the spinal cord. In a few spine specimens he found a cavity inside the spinal cord. Since the cavity had not been described before and had no name, he created the name syringomyelia by combining the Greek word syrinx meaning pipe, tube or channel, and the Greek word myelus, meaning marrow. Sixty-four years later, in 1891, Hans von Chiari, Professor of Morbid Anatomy at Charles University in Prague, published a report describing three cases with malformations of the lower part of the cerebellum and brain stem. Each of the three cases was different thus Chiari described three types of malformation: the type I, II, and III. Later, these malformations would be named the Chiari malformations in his honor.
The Chiari malformation Type I (CMI) consists of displacement (herniation) of the cerebellar tonsils into the upper cervical spinal canal. In some cases the lower brain stem also hangs down into the spinal canal. In the Type II malformation (almost always associated with spina bifida), the lower brain stem, cerebellar vermis, and tonsils hang down below the foramen magnum. In the very rare Type III malformation the tissues of the posterior fossa are displaced into a soft sac (meningocele) at the back of the head and upper neck. Dr. Chiari continued his studies and four years later published another report. In this one he described an additional 24 cases and made another important discovery. He found that some of the patients with the Chiari I and II malformations also had a cavity within the spinal cord – syringomyelia – the type of cavity that had been described by Charles Ollivier.
In the article, Dr. Chiari also reported a new type of malformation, Type IV, which consisted of underdevelopment of the cerebellum known as cerebellar hypoplasia. However, today we believe that the Type IV malformation is different from the other three and most specialists no longer include it within the Chiari classification.
Dr. Chiaris studies, performed over one hundred years ago, still serve as the foundation of our modern understanding of these malformations.
Diagnostic Studies: the MRI
Magnetic resonance imaging (MRI) has revolutionized neurological diagnosis. It gives detailed pictures of the brain, the spinal cord, and the surrounding tissues. When people without neurological symptoms undergo an MRI of the brain, the tonsils are found to be an average of 3 mm above the foramen magnum.
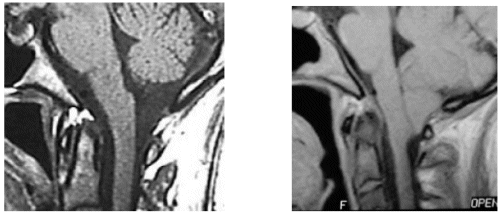 The figure above shows two MRI scans. The scan on the left is normal and shows cisterna magna. The tonsils are above the foramen magnum. The MRI on the right is that of a patient with the Chiari I malformation. The tonsils hang down below the foramen magnum and crowd out the cisterna magna, which is no longer visible. In this case, there is also a kink at the junction between the brain stem and spinal cord.
The figure above shows two MRI scans. The scan on the left is normal and shows cisterna magna. The tonsils are above the foramen magnum. The MRI on the right is that of a patient with the Chiari I malformation. The tonsils hang down below the foramen magnum and crowd out the cisterna magna, which is no longer visible. In this case, there is also a kink at the junction between the brain stem and spinal cord.
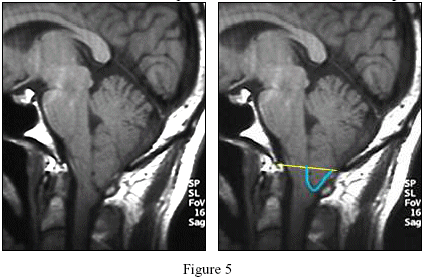 The Chiari I malformation is present when the tonsils herniate more than 3 or 5 mm below the foramen magnum. [see Figure 5] The measurement is taken by drawing a line from the end of the clivus bone (called the basion) to the end of the supraocciput (called the ophistheon). Another important finding is the amount of crowding at the foramen magnum.
The Chiari I malformation is present when the tonsils herniate more than 3 or 5 mm below the foramen magnum. [see Figure 5] The measurement is taken by drawing a line from the end of the clivus bone (called the basion) to the end of the supraocciput (called the ophistheon). Another important finding is the amount of crowding at the foramen magnum.
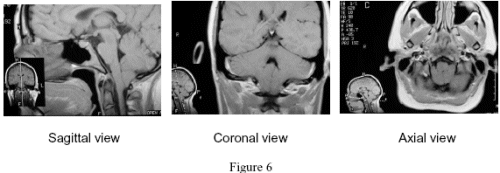
The MRI [see Figure 6] also allows one to see the posterior fossa in a side view (sagittal),
frontal view (coronal) and cross-sectional view (axial) as seen in these scans. In this case, they show herniation of the tonsils and crowding of the foramen magnum. No cisterna magna can be seen.
Twenty-five to 50% of people with the Chiari malformation also have signs that the bones of the skull or spine did not develop properly. The C1 vertebra, which is shaped like a ring, may not be completely formed, a condition called a bifid C1. In some cases, C1 is congenitally fused to the bottom of the skull, a condition called assimilation of C1. Other cases may have the upper part of the cervical spine indenting to some degree into the foramen magnum, a condition called basilar invagination. Another possibility is the fusion of two or more vertebrae of the spine, a condition called Klipple-Feil syndrome.
Pathophysiology
Many researchers believe that the Chiari malformation results from underdevelopment of the lower part of the skull. The posterior fossa is too small and does not provide the room needed for the cerebellum and the lower brain stem. Thus, the lower part of the cerebellum, and sometimes the lower part of the brain stem, develops below the foramen magnum. Why most people dont show symptoms in infancy is not well understood. What is known is that the brain moves with every heartbeat. Special MRI studies, called CINE MRI, have shown that the brain expands quickly with each heartbeat as blood is pumped into the brain. The briefly expanding brain, restricted by the fixed skull, moves downward toward the foramen magnum, which is already crowded in patients with the Chiari I malformation. This continuous downward pulsation of the brain can result in malfunction of the neurological tissue in the area. (On average, the heart beats 72 times each minute. Multiplying this by 60 minutes each hour and by 24 hours per day for 103,680 brain pulses per day!) Even worse, when a person with the Chiari I malformation coughs, sneezes or strains, there is additional downward pressure which causes the tonsils to impact into the foramen and cause an increase in the headache.
For most patients the Chiari malformation does not run in their family. However, in some cases it can pass down from the mother or father to son or daughter. Further research in this area may lead to a better understanding of the causes of the Chiari malformation.

Although the leading cause of syringomyelia is the Chiari malformation, it can also be caused by trauma, tumor, or infection. In some cases, the cause is unknown (idiopathic).
Figure 7 shows a large syrinx in the upper part of the spinal cord. It extends from just below the C1 level to C4
Symptoms of the Chiari I Malformation
Symptoms from the Chiari I malformation often develop in a slow and insidious manner. The symptoms are often vague and progress slowly over a number of years. Many patients have symptoms for years before they are diagnosed with the Chiari I malformation. About 1 out of 4 patients develop symptoms following trauma. The trauma is often mild or moderate in nature. Patients have reported accidents such as a fall from a trampoline, fall off a concrete porch, being hit on the back of head when a gas hose broke, or falling after hitting dog while riding a bicycle.
The most common symptom of the Chiari I malformation is headache. The headache usually begins at the back of the head and radiates behind one or both eyes, the top of the head or temples. The headache is often described as a pressure sensation but can be heavy, sharp, or stabbing. For many, the pain varies between these and other sensations. The headache is often made worse by straining activities (known as valsalva maneuvers) such as coughing, sneezing, or even laughing or singing. Some patients report feeling as though my head will explode or like my head will pop off. Bending forward, or looking up can worsen the headache. When the headache is intense, some patients will note dizziness, blurring of vision, nausea, or a feeling of a mental fog. A variety of other visual symptoms can occur with the Chiari I malformation including double vision, decreased peripheral vision, fireflies, visual loss, blind spots, photophobia, spasm of the eyelids (blepharospasm), and jerking of the eyes (nystagmus). Symptoms of the ears and the balance system include dizziness, ringing in the ears (tinnitus), poor balance (disequilibrium), decrease or loss of hearing, and vertigo. Other symptoms related to the cranial nerves and their nuclei include hoarseness, problems swallowing (dysphagia), slurring of words (dysarthria), and numbness of the face. Many patients complain of weakness, numbness or tingling, or pain in the arms or legs. Often, only one side is involved.
General symptoms include depression, poor sleep (insomnia) and fatigue. Some note problems with memory, thinking and speech. People report the feeling of a brain fog with difficulty in thinking and concentration. Difficulty in finding the right word is not uncommon.
Effects of the Chiari malformation on the respiratory and heart centers can cause shortness of breath, chest pain, episodes of rapid heart rate (tachycardia), black out spells, and hypertension. Abdominal symptoms may include nausea, abdominal pain, or vomiting.
With so many possible symptoms, most which can be caused by other conditions, a physician may not suspect the Chiari malformation as a possible cause of the symptoms. However, many patients seem to show a common pattern of symptoms as noted below.
Common pattern of symptoms:
- Occipital pressure headache, radiating forward, worse with valsolva
- Dizziness, often worse with headache or changing positions
- Transient blurring of vision, worse with HA
- Weakness of all or some extremities
- Pain or numbness in face or extremities
- Nausea
- Swallowing problems
- Chronic fatigue syndrome
- Fibromyalgia
- Sleep apnea
- Spinal CSF leak
- Arachnoid cyst
- Degenerative disc disease
- Psychiatric disease
- Migraine
- Cluster headache
- Rebound headache
- Pseudotumor cerebri
- Occipital neuralgia
- Post-concussion syndrome
- Hydrocephalus
- Multiple sclerosis
Treatment Options
Patients presenting with symptoms from the Chiari malformation often have received a variety of therapies. This can include medications such as analgesics, anti-inflammatories, sedatives, anticonvulsants, antispasmotics, diuretics, and steroids. Evaluation by a neurologist to evaluate for other neurological disorders is important.
Physical therapy may be of help in some patients and evaluation by a chronic pain specialist may be of help in others.
Surgical treatment of the Chiari malformation involves creating more space at the region of the foramen magnum to allow the spinal flow in this area to return toward normal. This is a done by a procedure called a posterior fossa decompression. The surgery is performed by creating an incision at the back of the head into the upper part of the neck. The muscles are spread to either side and the occipital bone and the back of the C1 vertebrae are visualized. Skull bone and often the arch of C1 (in some cases C2) are removed. Under the bone is a tough membrane called the dura. The surgeon then opens the dura. Here, the surgical technique varies depending on the practice of the surgeon. Some surgeons open the next layer called the arachnoid and may shrink the tips of the tonsils with electrocautery. Others do not open the arachnoid. Studies to date do not tell us which is best procedure. There is no documented untoward effect from shrinking the tonsils. The important point is to create more room and thus remove the crowding. Most surgeons will then sew a patch of material into the dura to enlarge the foramen magnum. The wound is then closed with stitches to bring the muscles together and stitches or staples on the skin.
There are some risks to surgery including pseudomeningocele (leak of spinal fluid through the membrane repair creating a fluid pocket in the muscle), infection, either in the wound or in the spinal fluid (meningitis), occipital neuralgia, and neurological deficit such as an injury, hemorrhage, or stroke. There are also the risks of any major surgery such as pneumonia, or cardiac problems.
In deciding whether to consider surgical treatment, the person affected by the Chiari I malformation should weigh the quality of their life versus what they understand about the possible benefits and risks. It is important to ask questions until one is comfortable with their understanding of the procedure, the possible benefits, and the associated risks.

